Fludarabine is an important anticancer drug used in the treatment of chronic lymphocytic leukemia (CLL) and non-Hodgkin lymphoma (NHL). Despite its significant efficacy, the use of fludarabine is also associated with a series of side effects, which may have a significant impact on patients' quality of life. Understanding fludarabine side effects and their management is crucial to ensure patient safety and improve treatment outcomes. This article will comprehensively explore the fludarabine side effects to assist patients and healthcare professionals in better addressing these challenges.
Injectable fludarabine is indicated for the treatment of adult patients with chronic B-cell lymphocytic leukemia (CLL) who have failed at least one standard alkylating-agent-containing regimen or have disease progression. The safety and efficacy of injectable fludarabine in previously untreated or non-refractory CLL patients have not been established. The structure of fludarabine is illustrated in the following diagram:

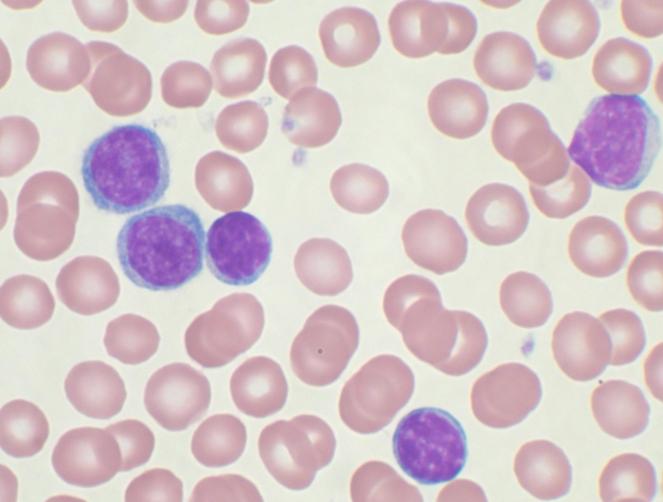
The very common adverse events include bone marrow suppression (neutropenia, thrombocytopenia, and anemia), fever and chills, fatigue, weakness, infections, pneumonia, cough, nausea, vomiting, and diarrhea. Other common events include discomfort, mucositis, and anorexia. CLL patients treated with injectable fludarabine experienced severe opportunistic infections (such as latent virus reactivation, herpes zoster virus, EB virus, and progressive multifocal leukoencephalopathy).
Fludarabine may cause fludarabine side effects, including:
- Measles
- Difficulty breathing
- Swelling of the face, lips, tongue, or throat
- Fever
- Chills
- Sore throat
- Flu-like symptoms
- Easy bruising
- Abnormal bleeding (nosebleeds, gum bleeding)
- Loss of appetite
- Nausea
- Vomiting
- Mouth ulcers
- Abnormal weakness
- Pallor or jaundice of the skin
- Dark urine
- Cough with yellow or green mucus
- Sharp chest pain
- Shortness of breath
- Black, tarry, or bloody stools
- Coughing up blood
- Lower back pain
- Blood in urine
- Decreased urination or no urination at all
- Numbness or tingling around the mouth
- Fast or slow heart rate
- Weak pulse
- Fainting
- Muscle weakness
- Tightness
- Contraction
- Excessive reflex activity
- Mood changes
- Increased thirst
- Swelling
- Rapid weight gain
- Vision problems
- Headache or pain behind the eyes
- Behavioral changes
- Confusion
- Agitation
- Seizures
- Severe blistering
- Red rash
If you experience any of the above symptoms, seek medical help immediately.
Common fludarabine side effects include:
- Nausea or vomiting (may be severe)
- Diarrhea
- Headache
- Muscle aches or pains
- Fatigue
- Loss of appetite
- Mouth ulcers
- Injection site reaction (pain or redness)
- Itching or rash
If you experience the following fludarabine side effects, seek medical attention or call emergency services immediately:
- Severe eye symptoms such as sudden vision loss, blurred vision, tunnel vision, eye pain or swelling, or seeing halos around lights;
- Severe heart symptoms such as fast, irregular, or pounding heartbeat; shortness of breath; sudden dizziness, lightheadedness, or fainting;
- Severe headache, confusion, difficulty speaking, weakness in the arms or legs, difficulty walking, loss of coordination, instability, very stiff muscles, high fever, profuse sweating, or tremors.
This article does not cover all possible side effects, and other side effects may occur. Consult your doctor for more information on fludarabine side effects.
Applicable to fludarabine: Injectable intravenous powder, intravenous solution, oral tablet.
Very common (10% or more): Neutropenia, anemia, thrombocytopenia.
Common (1%-10%): Bleeding, bone marrow suppression.
Very common (10% or more): Opportunistic infections (e.g., latent virus reactivation, progressive multifocal leukoencephalopathy, herpes zoster virus, EB virus) (44%).
Uncommon (0.1%-1%): Autoimmune diseases (e.g., autoimmune hemolytic anemia, Evans syndrome, idiopathic thrombocytopenic purpura, acquired hemophilia, pemphigus).
Rare (less than 0.1%): Lymphoproliferative disorders (EBV-related).
Very common (10% or more): Nausea/vomiting (36%), anorexia (34%), diarrhea (15%).
Common (1%-10%): Dehydration, stomatitis, gastrointestinal bleeding, esophagitis, mucositis, constipation, dysphagia.
Very common (10% or more): Weakness (69%), sensory abnormalities (12%).
Common (1%-10%): Headache, cerebellar syndrome, psychiatric disorders, peripheral neuropathy.
Rare (less than 0.1%): Coma, seizures.
Unreported frequency: Cerebral hemorrhage.
Very common (10% or more): Cough (69%), pneumonia (22%), dyspnea (22%), upper respiratory tract infection (16%).
Common (1%-10%): Sinusitis, pharyngitis, allergic pneumonia, epistaxis, hemoptysis, bronchitis, hypoxia.
Uncommon (0.1%-1%): Pulmonary toxicity (e.g., pulmonary fibrosis, pneumonia, dyspnea).
Unreported frequency: Pulmonary hemorrhage.
Very common (10% or more): Edema (19%).
Common (1%-10%): Angina pectoris, congestive heart failure, supraventricular tachycardia, myocardial infarction, deep vein thrombosis, phlebitis, transient ischemic attack, aneurysm, cerebrovascular accident.
Common (1%-10%): Urinary retention, urinary tract infection, hematuria, proteinuria, urinary hesitancy.
Common (1%-10%): Renal failure, abnormal renal function tests.
Common (1%-10%): Systemic allergic reactions.
Injectable fludarabine is a potent antineoplastic drug with potential significant toxic side effects. Close monitoring of hematological and non-hematological toxicity signs in patients undergoing treatment is advised. Regular assessment of peripheral blood counts is recommended to detect the occurrence of anemia, neutropenia, and thrombocytopenia.
In patients with compromised health status, caution should be exercised with the use of fludarabine, and risks/benefits should be carefully considered. This is especially applicable to patients with severely impaired bone marrow function (thrombocytopenia, anemia, and/or neutropenia), immunodeficiency, or a history of opportunistic infections. Prophylactic treatment should be considered for patients at increased risk of opportunistic infections.
Injectable fludarabine may impair the ability to drive or operate machinery, as fatigue, weakness, visual disturbances, confusion, agitation, and seizures have been observed.
Tumor lysis syndrome is associated with the treatment of injectable fludarabine. This syndrome has been reported in CLL patients with a large tumor burden. Due to the early induction of response with injectable fludarabine treatment, preventive measures should be taken for patients at risk of developing this complication.
Patients with renal impairment must be cautious with injectable fludarabine. Patients with a creatinine clearance of 30-79 mL/min should reduce the dose of fludarabine injection and monitor for excessive toxicity closely. Injectable fludarabine should not be used in patients with a creatinine clearance less than 30 mL/min.
For patients aged ≥65 years, creatinine clearance should be measured before starting treatment.
During treatment, patients' hematological characteristics (especially neutrophils and platelets) should be monitored regularly to determine the degree of hematopoietic suppression.
There are no animal carcinogenicity studies on injectable fludarabine.
Fludarabine can cause some long-term side effects, including an increased risk of other cancers, especially leukemia. It may also cause permanent damage to the bone marrow, affecting your body's ability to produce blood cells. It's important to discuss these potential long-term effects with your doctor if you're considering fludarabine treatment.
Fludarabine is primarily used to treat chronic lymphocytic leukemia (CLL), which is a cancer affecting white blood cells. In certain cases, it may also be used in combination with other drugs to treat other types of leukemia and lymphomas.
Delayed effects refer to fludarabine side effects that occur months or even years after fludarabine treatment. These effects may include secondary cancers, but also vision problems, hearing loss, and infections.
Fludarabine is known to cause neutropenia, which is a condition where the body produces too few white blood cells, particularly neutrophils, which are important for fighting infections. That's why regular blood tests are necessary when undergoing fludarabine treatment.
Fludarabine has significant efficacy in treating chronic lymphocytic leukemia and non-Hodgkin lymphoma, but fludarabine side effects should not be overlooked. Common side effects include bone marrow suppression, increased infection risk, neurological damage, and renal impairment. These side effects can severely impact patients' quality of life and treatment tolerance. Therefore, close monitoring of patients' health status, timely management, and alleviation of adverse reactions are essential when using fludarabine to ensure treatment safety and efficacy. By considering treatment outcomes and fludarabine side effects comprehensively, personalized treatment plans can maximize patient quality of life and treatment success rates. If you have any questions about the fludarabine side effects or need further information, be sure to consult your doctor.
[1]https://reference.medscape.com/drug/fludara-oforta-fludarabine-342217
[2]https://www.rxlist.com/fludara-drug.htm
[3]https://www.drugs.com/sfx/fludarabine-side-effects.html
[4]https://www.mayoclinic.org/drugs-supplements/fludarabine-oral-route/side-effects/drg-20072542?p=1
[5]https://en.wikipedia.org/wiki/Fludarabine
[6]https://go.drugbank.com/drugs/DB01073
 |
 |
 |