Fludarabine is a widely used chemotherapy drug for the treatment of hematologic malignancies, especially effective against chronic lymphocytic leukemia (CLL) and non-Hodgkin lymphoma (NHL). As a purine nucleoside analog, fludarabine disrupts DNA synthesis and repair, inhibiting cancer cell proliferation and growth. Its unique mechanism of action and significant efficacy make it an essential component of various hematologic malignancy treatment regimens. This article will provide detailed insights into the nature, mechanism of action, and clinical applications of fludarabine, facilitating a deeper understanding of this critical medication.
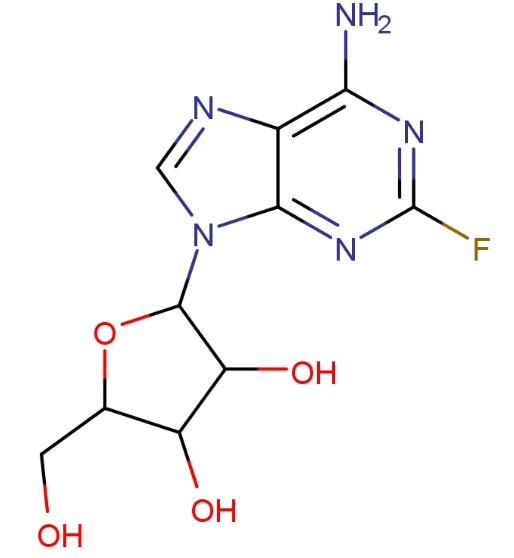
Fludarabine, also known as Fludara, is the systematic name for 9-β-D-arabinofuranosyl-2-fluoroadenine, with the molecular formula C10H12FN5O4. It is primarily used for the treatment of leukemia and lymphomas, including CLL, NHL, acute myeloid leukemia (AML), and acute lymphoblastic leukemia (ALL). Fludarabine is administered intravenously or orally and acts by interfering with DNA replication.
Fludarabine was approved for medical use in the United States in 1991 and is listed on the World Health Organization's List of Essential Medicines.
Fludarabine can be administered intravenously or orally in tablet form. For intravenous injection, healthcare professionals typically administer fludarabine over 30 minutes, with a recommended adult dose of 25 mg/m2. The infusion is given once daily for five consecutive days, with each 5-day course starting every 28 days.
For oral administration (tablets), the dosage for CLL is usually determined by the physician based on body surface area, with a typical dose of 40 mg/m2 once daily for five days, repeated every 28 days.
Fludarabine is a chemotherapy drug that interferes with DNA replication, thereby inhibiting the growth and proliferation of cancer cells. It belongs to a class of chemotherapy drugs known as antimetabolites.
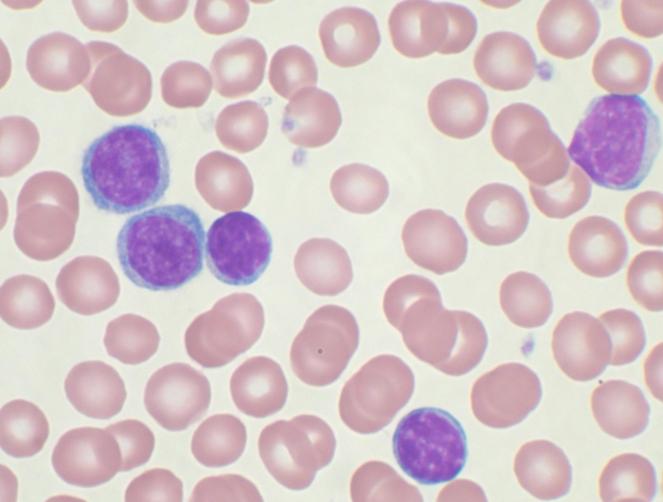
Fludarabine treatment is associated with severe lymphocytopenia, increasing the risk of opportunistic infections. Patients receiving fludarabine are often prescribed prophylactic medications to prevent infections. Severe lymphocytopenia can lead to transfusion-related graft-versus-host disease, a potentially fatal complication. Regular monitoring of blood cell counts is necessary to manage anemia, thrombocytopenia, and neutropenia. Some patients may require blood or platelet transfusions or injections of granulocyte colony-stimulating factor (G-CSF) to increase neutrophil counts.
Fludarabine may also cause autoimmune hemolytic anemia in some patients, and obtaining peripheral blood stem cells from previously treated patients may be challenging.
The frequency of fludarabine administration depends on the type of lymphoma or leukemia being treated. Treatment typically continues until there are minimal or no signs of abnormal leukemia or lymphoma cells in the blood. Treatment may be continued as long as the side effects are not too severe.
Blood tests are conducted before and during treatment to monitor blood cell levels and assess liver and kidney function. Dosing may be adjusted based on treatment response, and if adverse reactions occur, the dose may be reduced or treatment may be discontinued.
Side effects vary from person to person and depend on other treatments you are receiving. Healthcare providers will monitor potential side effects during treatment appointments. Early intervention can help better manage side effects.
Fludarabine is a crucial chemotherapy drug used primarily for treating CLL and NHL, among other hematologic malignancies. Despite its associated side effects, its contribution to delaying disease progression and improving patient survival rates cannot be overlooked. Close collaboration between physicians and patients is essential to ensure the effectiveness and safety of fludarabine treatment.
[1] Zhang K, Xu Y. Synthesis of antitumor drug fludarabine. Fine Chem Intermed. 2004; (04):33-35+41. DOI:10.19342/j.cnki.issn.1009-9212.2004.04.011.
[2]https://reference.medscape.com/drug/fludara-oforta-fludarabine-342217
[3]https://www.rxlist.com/fludara-drug.htm
[4]https://www.cancerresearchuk.org/about-cancer/treatment/drugs/fludarabine
[5]https://en.wikipedia.org/wiki/Fludarabine
 |
 |
 |