Medications within the same class may have various pharmacological characteristics, leading to significant differences in efficacy and tolerability in individual patients. For instance, β-blockers are a heterogeneous group of compounds with variations in adrenergic receptor selectivity, intrinsic sympathomimetic activity, and vasodilatory properties. These differences are reflected in their mechanisms of action and tolerability.
Metoprolol is a β1-selective blocker with a 74-fold higher preference for β1 receptors over β2 receptors. It is one of the most commonly used β-blockers for treating hypertension, and is the second most widely used antihypertensive medication overall. Since 2006, Metoprolol has been available as a generic drug in the U.S. Nebivolol, a more recently approved β-blocker for hypertension, is highly selective for β1 receptors (β1/β2 affinity ratio: 321) and exhibits nitric oxide (NO)-mediated vasodilatory effects. A meta-analysis of head-to-head randomized trials shows that Nebivolol has better tolerability compared to other β1-selective blockers, including Metoprolol. A retrospective claims analysis indicates that starting Nebivolol treatment is associated with a lower risk of discontinuation or switching to another antihypertensive drug compared to other β-blockers, including Metoprolol.
Nebivolol (Neb) is a third-generation β1 blocker with high selectivity for β1-adrenergic receptors and unique antioxidant properties, making it highly effective in treating hypertension. Nebivolol has unique characteristics not found in other β-blockers. For example, it enhances and promotes nitric oxide synthase, inducing nitric oxide-mediated vasodilation, reducing oxidative stress, dilating peripheral vessels, and improving endothelial vasodilation. Data also suggest that Nebivolol positively affects the fibrinolytic system, improving endothelial tissue plasminogen activator. Although β-blockers are not recommended as first-line therapy for primary hypertension, Nebivolol is an exception. Its high lipophilicity allows it to easily cross cell membranes, and its selectivity means it blocks β1 receptors with an intensity 300 times greater than β2 receptors, the highest among β-blockers. Nebivolol does not affect β2 receptors, avoiding bronchial and vascular smooth muscle contraction, and does not impact insulin sensitivity, while its intrinsic sympathomimetic activity ensures no negative stress effects.

Both Nebivolol and Metoprolol are β-blockers used for treating hypertension. They lower blood pressure by blocking the effects of adrenaline on β-receptors, reducing heart rate and dilating blood vessels. The main difference between Nebivolol and Metoprolol lies in their potency and dosing requirements.
A double-blind, multicenter parallel-group study compared the efficacy and safety of Metoprolol 100 mg twice daily and Nebivolol 5 mg once daily in 155 patients with mild to moderate hypertension. The study included an initial placebo phase followed by 3 months of active treatment. In the Nebivolol group, 79% of patients achieved normalized blood pressure, compared to 66% in the Metoprolol group. Adverse effects were fewer in the Nebivolol group, with only three patients on Metoprolol discontinuing treatment due to adverse effects. Nebivolol’s lower dose and once-daily administration improve patient compliance, which is particularly important for long-term hypertension management.
Why convert from Nebivolol to Metoprolol? The decision to switch from Nebivolol to Metoprolol is usually based on individual circumstances and medical needs. Potential reasons for this change include:
Lack of Effectiveness: If Nebivolol does not effectively control the patient's condition, such as hypertension or heart failure, other medications like Metoprolol may be considered.
Side Effects: Some individuals may experience adverse effects with Nebivolol, such as dizziness, fatigue, or bradycardia (slow heart rate). If these side effects are severe or interfere with daily life, switching to Metoprolol might be an option.
Drug Interactions: Nebivolol may interact with certain other medications. If a patient is taking drugs that negatively interact with Nebivolol, switching to Metoprolol may be necessary.
Individual Response: Each patient's response to medication is unique. If Nebivolol does not provide the expected results, Metoprolol may be considered.
Amlodipine, a CCB, can be used alone or in combination to treat hypertension and chronic stable angina and has been shown to have good safety. Its mechanism of action includes inhibiting calcium influx into vascular smooth muscle cells, thereby reducing peripheral vascular resistance.
Nebivolol combined with Amlodipine is primarily used to treat hypertension. Amlodipine works by relaxing blood vessels, while Nebivolol dilates vessels and makes it easier for the heart to pump blood throughout the body.

Transitioning from Nebivolol to Metoprolol requires a carefully planned conversion to minimize adverse effects. Individual responses may vary, and adjustments may be necessary. It is crucial to consult healthcare professionals to determine the most appropriate conversion ratio based on specific factors such as patient health status, history, and current dosage. Nebivolol can be taken with or without food, in tablet form, with a daily oral dose of 5-40 mg. Metoprolol tartrate (Lopressor) is dosed at 100-450 mg daily, while Metoprolol succinate (Toprol XL) ranges from 25-100 mg (initial dose) to 100-400 mg (maintenance dose).
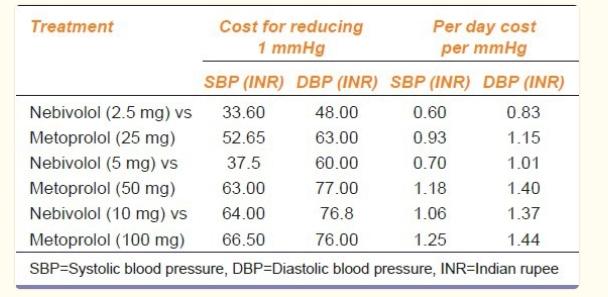
Rachna S. Patel et al. compared the cost-effectiveness of Nebivolol and extended-release Metoprolol in lowering blood pressure in hypertensive patients. The cost per pill of Nebivolol at 2.5 mg daily is 4.80 INR, while that of extended-release Metoprolol at 25 mg daily is 4.50 INR. Cost comparisons showed that Nebivolol had a lower cost per mmHg reduction in systolic and diastolic blood pressure compared to Metoprolol, especially at lower equivalent doses. The cost for reducing blood pressure in different dosing regimens of Nebivolol versus Metoprolol is outlined in the table below:
Close monitoring throughout the conversion process is essential to ensure patient safety and effectiveness. Healthcare providers should regularly assess blood pressure, heart rate, and overall cardiovascular function. Patients should report any unusual symptoms such as dizziness, fatigue, or shortness of breath. If adverse effects occur, adjustments to the Metoprolol dosage may be necessary. Maintaining open communication with the healthcare team is crucial to address any issues and optimize the transition to Metoprolol.
When converting from Nebivolol to Metoprolol, careful management is essential to ensure safety and effectiveness. Although both drugs are β-blockers, they differ in potency and mechanisms, making a straightforward conversion not feasible. Factors such as the patient’s specific health condition, current dosage, and potential side effects should be considered. For the best treatment outcomes and to avoid potential side effects, it is strongly recommended to consult a physician before making any medication changes and to follow their guidance for adjustments. Physicians will provide personalized advice based on the patient’s condition to ensure a smooth and safe transition.
[1]https://link.springer.com/article/10.1007/BF03258273
[2]https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4175882/
[3]https://pubmed.ncbi.nlm.nih.gov/14593370/
[4]https://www.tandfonline.com/doi/full/10.1080/03007995.2024.2328652
[5]https://onlinelibrary.wiley.com/doi/10.1002/ehf2.12153
[6]https://www.drugs.com/compare/metoprolol-vs-nebivolol
[7]https://en.wikipedia.org/wiki/Nebivolol
[8]Di Shiwei. Study on separation of key chiral intermediates of nebivolol by preparative chromatography[D]. Shanghai Jiaotong University, 2018.DOI:10.27307/d.cnki.gsjtu.2018.002896.
 |
 |
 |