
Nebivolol is a beta-blocker used to treat hypertension and heart failure. Although it is an effective treatment option, it is not usually the first choice for hypertension. Nebivolol can be used alone or in combination with other antihypertensive drugs to improve efficacy. It is available in an oral form, making it easier for patients to take.
Nebivolol was patented in 1983 and entered medical use in 1997. It is available as a generic drug in the United Kingdom. In 2021, it was the 244th most commonly prescribed drug in the United States, with more than 1 million prescriptions.
Carvedilol, sold under the brand name Coreg, is a beta-blocker used primarily to treat hypertension and chronic heart failure with reduced ejection fraction (HFrEF or systolic heart failure). Although carvedilol is effective in the management of these conditions, beta-blockers are not generally recommended as the first choice for all patients with hypertension. Studies have shown that beta-blockers are less effective and less safe than other blood pressure lowering drugs in terms of cardiovascular protection, and therefore should not be used as a routine first-line treatment option.
Carvedilol was patented in 1978 and approved for medical use in the United States in 1995. It is on the World Health Organization's list of essential medicines. It is available as a generic drug. In 2021, it was the 26th most commonly prescribed drug in the United States, with more than 21 million prescriptions.

Nebivolol and carvedilol are both third-generation β-blockers with vasodilatory effects. Carvedilol is a non-selective β-blocker with additional α1-blocking and antioxidant properties. Nebivolol is a selective β-1 adrenergic blocker with nitric oxide-dependent vasodilation and antioxidant effects.
Okan Erdo?an et al. compared the antihypertensive effects of carvedilol and nebivolol in patients with mild to moderate hypertension. This was a prospective, placebo-controlled, crossover, double-blind, randomized, single-center clinical trial. Patients newly diagnosed with mild to moderate systemic hypertension (mean ambulatory blood pressure > 130/85 mmHg) and who had not previously received antihypertensive treatment (n=20) were included in the study. After a 10-day placebo run-in period, they were randomly assigned to receive either carvedilol 25 mg or nebivolol 5 mg for one month each, administered once daily. The primary outcome measures were systolic and diastolic blood pressure determined by 24-hour ambulatory blood pressure monitoring. Statistical analysis using a 3x2 factorial repeated measures ANOVA showed that both carvedilol and nebivolol effectively lowered blood pressure compared to placebo, with similar antihypertensive efficacy.
Heart failure (HF) is a condition prevalent among the elderly, with up to 50% of HF diagnoses and 90% of HF deaths occurring in individuals over 70 years of age. Additionally, a significant portion of elderly HF patients have preserved systolic function, with poor prognosis comparable to that of HF with reduced ejection fraction. Therefore, diagnosing and treating HF with preserved ejection fraction (EF) is crucial. Diastolic dysfunction leads to elevated left ventricular filling pressures at rest or during exertion, worsening dyspnea, impairing exercise capacity, and reducing survival rates in patients with HF with preserved EF. β-blockers are thought to improve diastolic dysfunction through their negative chronotropic effects. A previous retrospective observational study indicated that seven years of long-term β-blocker use could improve left ventricular diastolic function in patients with HF with preserved EF. Recently, carvedilol and nebivolol, as third-generation β-blockers with vasodilatory effects, have been introduced into practice.
β-blockers can improve left ventricular (LV) systolic function and prognosis in chronic heart failure (CHF) patients, but their differing pleiotropic effects may impact their cardiovascular actions. Giuseppe Marazzi et al. compared the effects of long-term nebivolol vs carvedilol treatment on left ventricular ejection fraction (LVEF) in hypertensive CHF patients. Secondary endpoints included assessing the impact of the two β-blockers on exercise capacity and clinical outcomes. A total of 160 hypertensive CHF patients with LVEF <40% and New York Heart Association (NYHA) functional class I, II, or III were randomly assigned to receive either nebivolol or carvedilol for 24 months. Long-term, nebivolol and carvedilol appear to have comparable efficacy in treating hypertensive patients with congestive heart failure.
Common side effects of nebivolol include dizziness, fatigue, nausea, and headaches. Serious side effects may include heart failure and bronchospasm. It is not recommended for use during pregnancy and breastfeeding.
Common side effects of carvedilol include dizziness, fatigue, joint pain, hypotension, nausea, and shortness of breath. Serious side effects may include bronchospasm. Safety during pregnancy or breastfeeding is unclear, and it is not recommended for individuals with liver issues.
It is generally recommended to use only one β-blocker at a time. In some cases, the benefits of using such a drug combination may outweigh the risks. Always consult your healthcare provider before changing your medication or dosage.
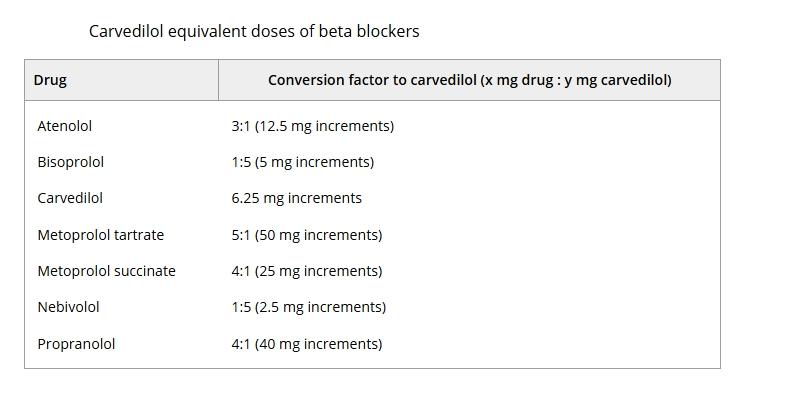
Alain Cohen-Solal et al. submitted β-blocker dosage data from 707 participants. Data from another 73 participants were obtained through record reviews. The β-blockers used by the 780 study subjects were as follows: carvedilol: 438, metoprolol: 211, bisoprolol: 99, atenolol: 28, nebivolol: 3; propranolol: 1. Use the factors shown in the table to convert β-blocker doses to carvedilol-equivalent doses:
Both nebivolol and carvedilol are commonly used antihypertensive medications, but they differ in mechanisms, side effects, and other aspects. The suitability of either medication depends on your specific condition, physical status, and medication history. Therefore, always use medications under the guidance of a physician. Medication use involves professional knowledge, so consult your doctor with any concerns.
 |
 |
 |